Three-Person DNA Technique Produces Healthy Babies in Britain
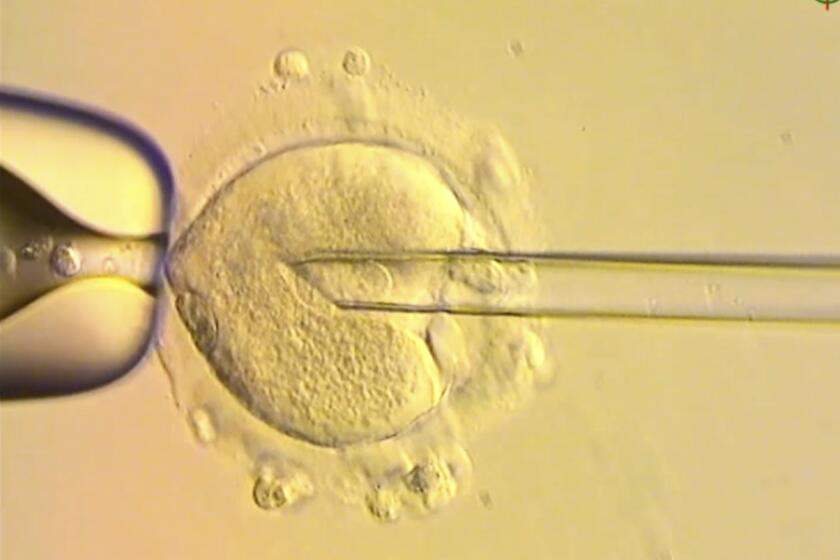
Breakthrough in Mitochondrial Replacement Therapy
A groundbreaking development in reproductive medicine has led to the birth of eight healthy babies in Britain, using an experimental technique that involves DNA from three people. This method aims to prevent mothers from passing on rare and devastating mitochondrial diseases to their children, according to recent research.
Mitochondria, often referred to as the powerhouses of the cell, contain a small amount of DNA separate from the genetic material found in the nucleus. While most of our DNA is inherited from both parents, mitochondrial DNA comes exclusively from the mother. Mutations in this DNA can lead to severe conditions such as muscle weakness, seizures, developmental delays, and even organ failure. In some cases, these mutations are not detectable through standard in vitro fertilization testing, leaving families with few options.
To address this issue, scientists have developed a technique known as mitochondrial replacement therapy. This approach involves replacing the mitochondria from a donor egg with the mother's genetic material. The process was first reported in 2023, with the birth of the first babies using this method. It requires a legal framework, which was established in the United Kingdom in 2016, allowing for the use of this technique under strict regulatory oversight.
The latest study, published in the New England Journal of Medicine, details how researchers at Newcastle University in Britain and Monash University in Australia used this method on 22 patients. As a result, eight babies were born without mitochondrial diseases, while one woman remains pregnant. Although one baby showed slightly higher levels of abnormal mitochondria, experts believe the risk is low and will be monitored closely as the child develops.
Dr. Zev Williams, director of the Columbia University Fertility Center, praised the advancement, calling it an important milestone in reproductive medicine. He emphasized that expanding reproductive options empowers couples to pursue safe and healthy pregnancies. However, he also noted that the technique is still limited to a small number of cases where other methods, such as embryo screening, are not viable.
Robin Lovell-Badge, a scientist at the Francis Crick Institute, highlighted that the DNA contributed by the mitochondrial donor is minimal—less than 1% of the total genetic material. He compared this to bone marrow transplants, which involve a much larger share of foreign DNA but do not raise similar concerns about heritable traits.
In the UK, all couples seeking to use donated mitochondria must receive approval from the country’s fertility regulator. To date, 35 patients have been authorized to undergo the procedure. Despite its success, the technique remains controversial, with critics warning about potential long-term effects on future generations.
In the United States, mitochondrial replacement therapy is not permitted for clinical use due to regulatory restrictions. The Food and Drug Administration is prohibited from accepting applications for research involving heritable genetic modifications. However, advocates argue that the technique could offer hope to families affected by mitochondrial diseases.
Liz Curtis, a mother who lost her daughter Lily to a mitochondrial disease, has become an advocate for research into these conditions. She described the emotional impact of receiving a diagnosis with no available treatment. Her efforts led to the creation of the Lily Foundation, which supports families and funds research into mitochondrial diseases.
For many families, this breakthrough represents a new hope. As scientific advancements continue, the ethical and regulatory landscape surrounding such techniques will likely evolve, shaping the future of reproductive medicine.
Post a Comment for "Three-Person DNA Technique Produces Healthy Babies in Britain"
Post a Comment