Caremark's PBM Leadership in CalPERS' Vision: What's on the Line?
Rising Prescription Drug Costs and the Role of PBMs
Prescription drug costs continue to be a major concern for patients and healthcare providers alike, with pharmacy benefit managers (PBMs) under increasing scrutiny for their influence on drug pricing and coverage. These entities play a crucial role in managing prescription drug benefits for insurers and health plans, making their decisions impactful on both cost and access.
CVS Health’s CVS Caremark division recently secured a significant contract with The California Public Employees’ Retirement System (CalPERS), which is the largest public pension fund in the United States. This five-year agreement replaces OptumRx, the PBM arm of UnitedHealth Group, which had been serving CalPERS members for nearly a decade. Starting January 1, 2026, Caremark will provide outpatient prescription drug benefits to approximately 587,000 members enrolled in Basic or Medicare HMO and PPO plans, covering roughly 40% of CalPERS’ total 1.5 million beneficiaries.
In addition to this, CVS Caremark will collaborate closely with CalPERS to develop options for managing formulary changes that could impact copays or require switching to equally effective alternatives. The selection of CVS was based on its ability to deliver more affordable drug benefits and its commitment to strong contract terms focused on accountability, transparency, and innovative financial guarantees. As part of the agreement, CVS has put $250 million at risk if it fails to meet targets for controlling pharmacy benefit costs and delivering clinical quality outcomes tied to improving care for conditions like high blood pressure and diabetes.
This partnership positions CVS Caremark as a key player in CalPERS’ efforts to create a model that can serve as a blueprint for other purchasers nationwide. It highlights the growing importance of PBMs in shaping the future of prescription drug coverage and affordability.
Strategic Moves by CVS Health
This year, CVS Health made a strategic decision to prefer Wegovy over Zepbound on its commercial template formularies. This move aims to promote competition in reducing drug costs and enable broader, more affordable coverage for weight management medications. As a result, clients using CVS Caremark’s template formularies could save between 10-15% annually in the anti-obesity medication space.
Updates from PBM Peers
The global PBM market is expanding, with CVS Caremark, OptumRx, and Express Scripts (Cigna) leading the way. Other notable players include Elevance Health, which operates through its CarelonRx unit. Recent earnings reports show that CarelonRx experienced a 33% year-over-year increase in operating gains, driven by higher prescription volumes and recent acquisitions.
Humana also operates a PBM business within its Insurance segment. Recently, Humana announced a partnership with Epic, becoming the first health insurer to integrate health plan information directly into MyChart accounts. This allows Humana Medicare Advantage members to access their insurance details, including vital coverage information, benefits, contacts, and other resources, all in one platform where they manage their overall care.
Financial Performance and Valuation
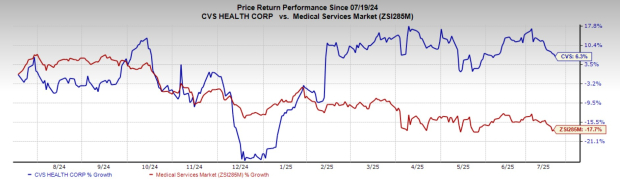
Over the past year, CVS Health shares have increased by 6.3%, outperforming the industry's 17.7% decline. Currently, CVS shares are trading at a forward one-year price-to-earnings ratio of 9.60, compared to the industry average of 14.00. The stock carries a Value Score of A, indicating strong investment potential.
Analyst estimates for CVS Health’s 2025 and 2026 earnings are showing an upward trend. Additionally, the stock currently sports a Zacks Rank of #1 (Strong Buy), reflecting positive expectations for future performance. Investors interested in exploring other top-ranked stocks can refer to the complete list of today’s Zacks #1 Rank stocks.
Post a Comment for "Caremark's PBM Leadership in CalPERS' Vision: What's on the Line?"
Post a Comment