Understanding Stable Blood Glucose Protocols: A Comprehensive Guide
Maintaining stable blood glucose levels is one of the most critical aspects of overall health, especially for individuals with diabetes or those at risk of developing it. Whether you're managing a chronic condition or simply looking to improve your well-being, understanding and implementing effective blood glucose protocols can make a significant difference in your quality of life. This article will explore what stable blood glucose means, why it matters, and how to achieve it through diet, lifestyle, and medical support.
What Is Stable Blood Glucose?

Stable blood glucose refers to maintaining consistent and healthy levels of sugar (glucose) in the bloodstream throughout the day. For most people, this means keeping blood sugar within a target range that avoids both high (hyperglycemia) and low (hypoglycemia) spikes.
For individuals without diabetes, blood glucose typically fluctuates between 70–140 mg/dL depending on when they last ate. However, for those with diabetes, maintaining stability is more complex due to issues with insulin production or function. The goal is to prevent extreme swings that can lead to complications such as fatigue, mood changes, and long-term damage to organs and nerves.
Why Blood Sugar Stability Matters

The importance of stable blood glucose extends beyond just avoiding immediate symptoms like dizziness or irritability. Chronic instability can lead to serious health issues, including:
- Heart disease: High blood sugar levels can damage blood vessels and increase the risk of heart attacks and strokes.
- Kidney disease: Prolonged hyperglycemia can impair kidney function, potentially leading to failure.
- Neuropathy: Uncontrolled blood sugar can cause nerve damage, resulting in pain, tingling, or numbness, particularly in the hands and feet.
- Vision problems: Diabetes is a leading cause of blindness due to damage to the retina.
Even for those without diabetes, maintaining stable glucose levels can enhance energy, focus, and mood regulation. It also reduces the risk of developing type 2 diabetes in the future.
Key Components of Stable Blood Glucose Protocols

Achieving and maintaining stable blood glucose involves a combination of dietary choices, physical activity, and, in some cases, medication. Here are the essential elements of an effective protocol:
1. Balanced Diet
A well-planned diet is foundational to blood glucose control. Focus on foods that are high in fiber, protein, and healthy fats while limiting refined carbohydrates and added sugars. Some top choices include:
- Beans and lentils – Rich in fiber and plant-based protein, which help slow digestion and reduce blood sugar spikes.
- Seafood – Especially oily fish like salmon and mackerel, which are high in omega-3 fatty acids and may improve insulin sensitivity.
- Avocados – Loaded with monounsaturated fats and magnesium, which support healthy blood sugar regulation.
- Greek yogurt – High in protein and probiotics, which can improve gut health and insulin response.
- Chia seeds – Packed with fiber and magnesium, these tiny seeds help regulate blood sugar and support pancreatic function.
- Nuts and seeds – Provide healthy fats, protein, and minerals that aid in stabilizing glucose levels.
Avoiding sugary drinks, white bread, and processed snacks is equally important. These foods can cause rapid spikes in blood sugar, making it harder to maintain balance.
2. Regular Physical Activity

Exercise plays a crucial role in blood glucose management by improving insulin sensitivity and increasing the body's ability to use glucose effectively. Aim for at least 150 minutes of moderate-intensity aerobic activity per week, such as walking, cycling, or swimming. Strength training is also beneficial, as it helps build muscle mass, which can enhance glucose uptake.
3. Monitoring and Adjustments

Regular monitoring of blood glucose levels allows for early detection of fluctuations and enables timely adjustments to diet, exercise, or medication. Continuous glucose monitors (CGMs) are becoming increasingly popular for real-time tracking, while traditional finger-prick tests remain a reliable option for many.
4. Medication and Insulin Therapy
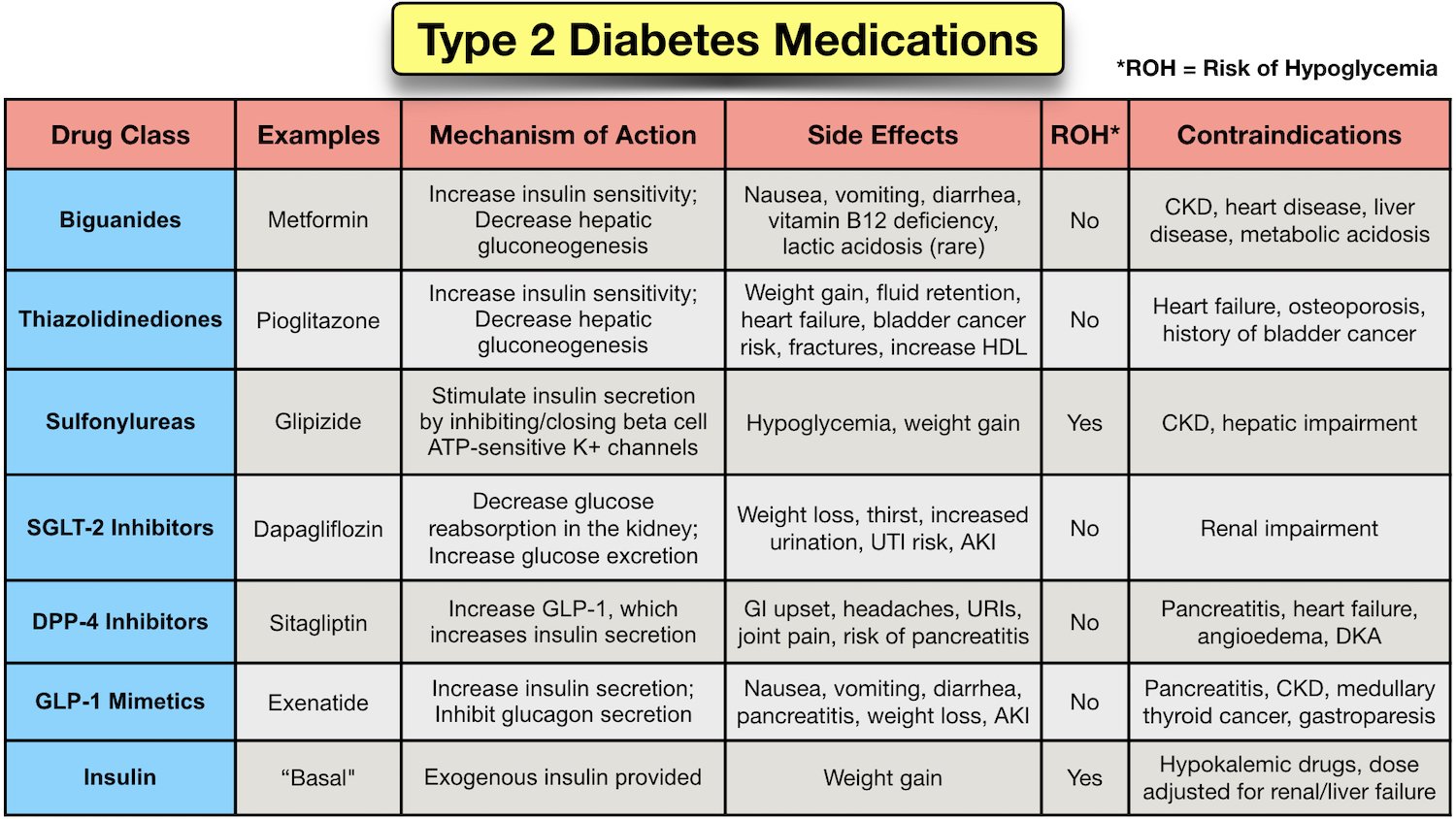
For individuals with diabetes, medications such as metformin, GLP-1 receptor agonists, and SGLT2 inhibitors can be used to manage blood sugar levels. Insulin therapy may also be necessary for those who cannot control their glucose through lifestyle changes alone. Always follow your healthcare provider’s guidance when using these treatments.
Practical Tips for Maintaining Stable Blood Glucose

Here are some actionable strategies to help you implement stable blood glucose protocols effectively:
- Eat regular, balanced meals – Avoid skipping meals, as this can lead to overeating later and cause blood sugar spikes.
- Pair carbs with protein and fat – Combining high-carb foods with protein or healthy fats slows digestion and prevents sharp increases in blood sugar.
- Stay hydrated – Drinking enough water helps flush out excess glucose and supports overall metabolic function.
- Limit alcohol intake – Alcohol can cause unpredictable changes in blood sugar levels, so it’s best to consume it in moderation and always with food.
- Prioritize sleep – Poor sleep can disrupt hormonal balance and increase insulin resistance. Aim for 7–9 hours of quality sleep each night.
Conclusion
Stable blood glucose protocols are essential for anyone looking to maintain optimal health, whether they have diabetes or not. By focusing on a balanced diet, regular exercise, and proper monitoring, individuals can significantly reduce the risk of complications and enjoy improved energy and well-being. Remember, consistency is key—small, sustainable changes over time can lead to lasting results. If you’re unsure where to start, consult with a healthcare professional or registered dietitian to create a personalized plan that works for you. Your journey to stable blood glucose begins with knowledge, and now you have the tools to take the next step.

Post a Comment for "Understanding Stable Blood Glucose Protocols: A Comprehensive Guide"
Post a Comment